From credentialing and payer enrollment to billing and AI-powered denial intelligence, VANAA handles the full revenue cycle so your in-house team can stop stressing about backlogs.
VANAA operates as an extension of your teams! Or becomes your ONLY team. Every workflow is augmented by AI - from exception handling, pattern detection, to claim optimization and more.
Live Updates And Queries
Multiple Project Managers
AI-Powered Analytics
Independent Quality Team
Outsourcing Without Lock-In
Human Scale Augmented With AI
Whether you need to onboard a new provider or recover revenue that’s slipping through denials, we’ve built the process, the technology, and the team for both.
Credentialing is complex, payer-specific, and painfully easy to get wrong, and the consequences land directly on your cash flow.
VANAA handles provider credentialing, payer enrollment with Medicare, Medicaid, and commercial insurers, CAQH setup and attestation, re-credentialing, and multi-state licensing, with full status transparency throughout.
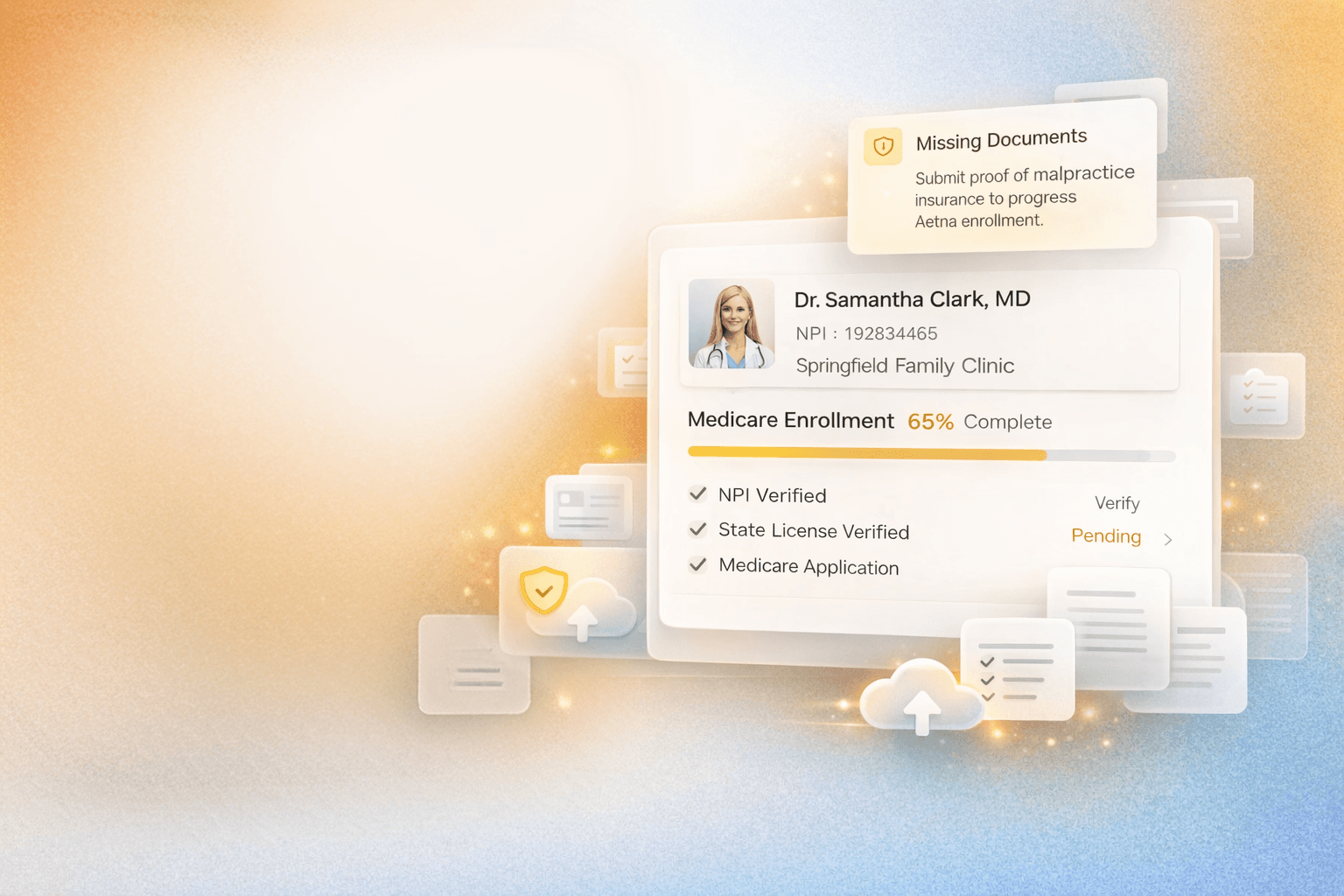
Credentialing is complex, payer-specific, and painfully easy to get wrong, and the consequences land directly on your cash flow.
VANAA handles provider credentialing, payer enrollment with Medicare, Medicaid, and commercial insurers, CAQH setup and attestation, re-credentialing, and multi-state licensing, with full status transparency throughout.

A claim submitted is not a claim paid. Between errors in eligibility & coding, payer-specific rule changes, denials, and aging AR buckets, most practices are leaving significant revenue on the table without realizing it.
VANAA manages the full cycle: eligibility, authorizations, charge entry, medical coding, claims submission and scrubbing, denial management, AR follow-up, patient billing, and analytics, with AAPC-certified coders and AI-powered denial intelligence built in.
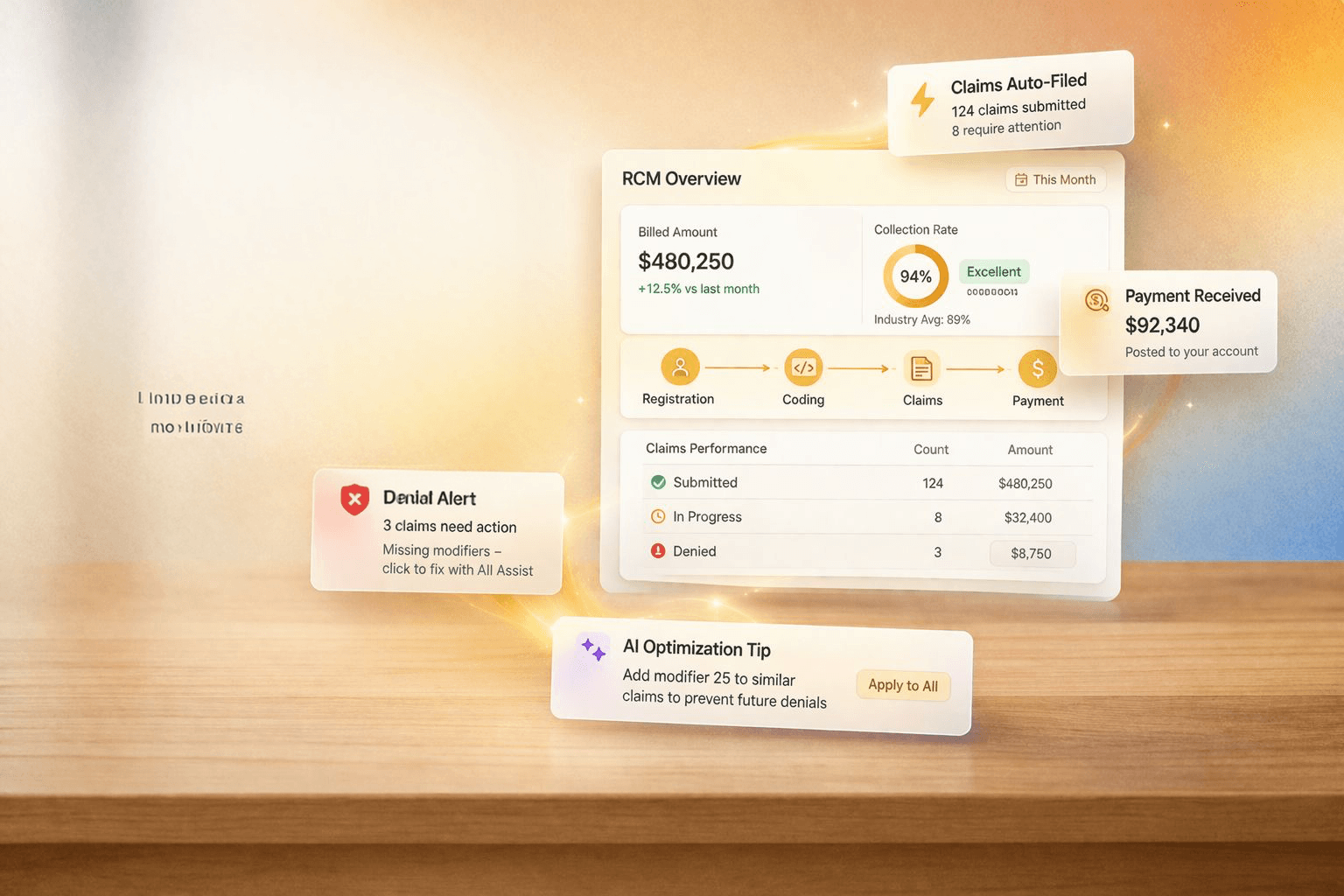

A claim submitted is not a claim paid. Between errors in eligibility & coding, payer-specific rule changes, denials, and aging AR buckets, most practices are leaving significant revenue on the table without realizing it.
VANAA manages the full cycle: eligibility, authorizations, charge entry, medical coding, claims submission and scrubbing, denial management, AR follow-up, patient billing, and analytics, with AAPC-certified coders and AI-powered denial intelligence built in.
End-to-end credentialing, enrollment, and revenue cycle management, bundled, AI-augmented, and running on autopilot. No supervision. No inputs. No surprises.
Applications submitted first-time-right within 24 hours.
Repeat denial patterns stopped cold by the VAN-DRA™Engine [Denial Reason Analytics].
Denials prevented before they’re filed, not chased after.
Recoveries automated. Rejections don’t sit, they resolve.
Audit-ready 24/7, no scrambling when payers ask.
Regulatory updates weekly, built into your workflow with your permission.
Zero compliance surprises across multi-state, multi-specialty operations.
Add providers without adding headcount with us.
Credential across states without process breakdowns.
Revenue cycle expands with your organization, not against it.
When automation handles the routine, speed becomes a natural outcome.
Get a No Cost No Obligation Consultation
Automated workflows cut financial administrative workloads by up to 50%, so your team focuses on patients, not paperwork.
Proactive, audit-ready operations that minimize claim denials and safeguard revenue before issues surface.
Up to 20% higher profitability, without compromising compliance or patient satisfaction.

We Simplify Healthcare Operations for You.
Medicare, Medicaid and Private Commercials plus LOBs including HMOs, PPOs etc.










































Every specialty has its own coding nuances, payer quirks, and compliance landmines. we’ve worked across many of them so you don’t have to explain yours from scratch.
Every specialty has its own coding nuances, payer quirks, and compliance landmines. we’ve worked across many of them so you don’t have to explain yours from scratch.





At Pure Psychiatry Group and ACPC, we are pleased to provide our strong endorsement of Vanna RCM for their exceptional revenue cycle management and credentialing services. Since partnering with Vanna RCM, including their credentialing department, we have experienced significant improvements in both our billing operations and provider onboarding processes. Their team consistently demonstrates a high level of expertise, accuracy, and responsiveness in managing claims, reducing denials, accelerating reimbursements, and ensuring timely and efficient credentialing with payers. As a result, our organization has seen measurable improvements in cash flow, operational efficiency, and speed to service for new providers. Vanna RCM’s proactive approach and deep understanding of behavioral health billing and credentialing, including Medicaid and commercial insurance, have made them a valuable and trusted partner. We highly recommend Vanna RCM to any healthcare organization seeking a reliable and knowledgeable revenue cycle and credentialing partner.
Bridgette Trader
Revenue Cycle Management Director Pure Psychiatry Group and ACPC
VANAA delivers Provider Licensure, Credentialing, and Payer enrollment services with flexible maintenance models.
VANAA delivers End-to-end Revenue Cycle Management (RCM) or customized service modules for Charge Entry, Medical Coding, Billing, Denial Management, and Revenue Analytics. Our automation-first workflows have helped practices cut denials by 22%+ and improve net collections by upto 25%+ within 4 months.
VANAA's services are designed for a wide range of healthcare providers — from solo practitioners and small group practices to large multi-specialty clinics and hospital systems.
Whether you're a physician, dentist, chiropractor, behavioral health provider, or any other specialist, VANAA's revenue cycle solutions are tailored to your unique billing requirements and payer mix.
VANAA operates in full compliance with HIPAA, HITECH, and all applicable federal and state regulations. Our systems are protected with end-to-end encryption, role-based access controls, and continuous security audits.
We maintain SOC 2 Type II standards and conduct regular risk assessments to safeguard your patient data and practice information at every touchpoint in the revenue cycle.
Practices partnering with VANAA typically see measurable financial improvements within the first 90 days. On average, our clients experience a 22%+ reduction in claim denials and up to 25%+ increase in net collections.
Our team works proactively to identify revenue leakage, accelerate reimbursements, and optimize every stage of your billing workflow — resulting in a 30–40% faster payment cycle.
Yes — VANAA integrates seamlessly with all major Electronic Health Record (EHR) and Practice Management System (PMS) platforms, including Epic, Athenahealth, eClinicalWorks, Kareo, DrChrono, and more.
Our onboarding team handles the full integration setup, data migration, and staff training so your practice experiences zero downtime during the transition.